Rhinoscopy can be a life-saving diagnostic tool...
This site provides allergists with critical information and guidance concerning the flexible rhinolaryngoscope and how to best make use of it in practice.
Anterior rhinoscopy using otoscopes with nasal speculum attachments provide only a keyhole perspective of the anterior nose. Flexible endoscopy however allows examination of the entire nasal cavity and more distal anatomy. It is most commonly performed by otolaryngologists in the evaluation of nasal obstruction, sinusitis, epistaxis, anosmia, other symptoms of rhinitis, and head and neck cancer. It can also be performed by allergists in the evaluation of the upper airway. Flexible rhinoscopy is commonly performed with no specific pre-procedure restrictions or contraindications. With practice and experience, the office-based procedure takes only a few minutes and is well tolerated by the majority of patients.
| Important Upper Airway Structures | |
|---|---|
The major passages and structures of the upper respiratory tract include the nose or nostrils, nasal cavity, mouth, throat (pharynx), and voice box (larynx).
|
| Technique of Examination | |
|---|---|
The physician interested in extending his knowledge of the nose, the pharynx, and the larynx can use fiberoptic rhinoscopy for examination of virtually all patients with upper airway complaints. There are, of course, certain limitations when it comes to examination of children, but with a reassuring bedside manner, proper and safe restraint techniques, and judicious use of analgesics, amnesics and sedatives, examination of even very small children can be accomplished.
|
| Upper Airway Pathology | |
|---|---|
The differential diagnoses of nasal obstruction include both anatomic, inflammatory, and infectious causes. Anatomic causes identifiable through nasal endoscopy include nasal polyps, nasal valve collapse, septal deviation/perforation, synechiae, and turbinate hypertrophy. Nasal or sinus tumor may occur as well, of course, but fear of missing this diagnosis should not preclude the attempt. Sources of inflammation and infection can also be predicted. Thorough history, including chronic illnesses, past surgeries, current medications, onset, duration, and aggravating/relieving factors, can help to narrow the differential diagnoses.
|
| Coding and Reimbursement |
|---|
|
| Resources |
|---|
| This set of resources comes from the Introductory Course in Rhinolaryngoscopy by Jerald W. Koepke, MD. |
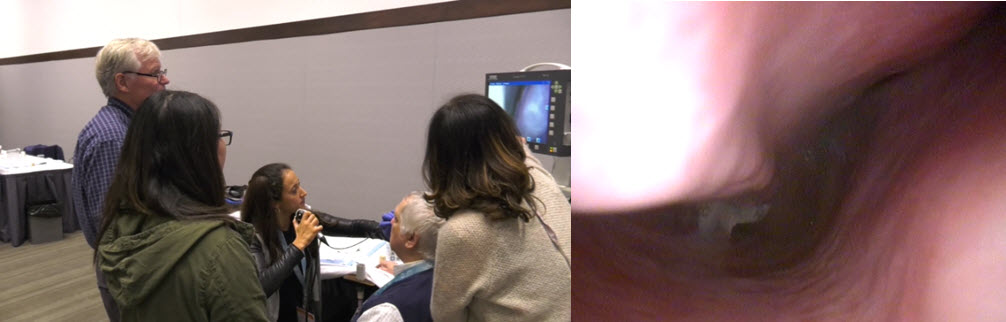
Attendees practice using a rhinolaryngoscope during the ACAAI annual meeting
| Ask an Expert: Your Rhinolaryngoscopy Questions Answered | |
|---|---|
Q: Should an allergist who is treating children, consider using the rhinoscope as a diagnostic tool in young children? | |
| Have a question for the experts? Let us know and we will post a response! |

 Facebook
Facebook X
X LinkedIn
LinkedIn Forward
Forward